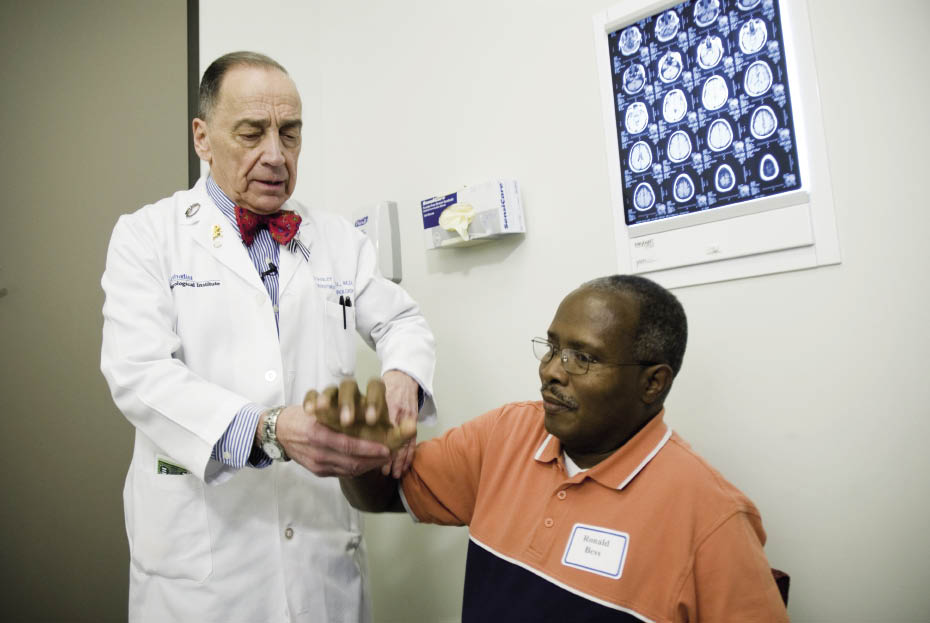
It takes a village Multidisciplinary care can improve the quality of life and survival of people with ALS according to experts at AAN 2014. Image courtesy of Stanley Appel MD.
More than 30 potential therapies for ALS are currently being tested in the clinic. A growing number of repurposed medicines including immunomodulators Actemra, Gilenya and Proleukin are entering at the phase II stage. A phase IIB clinical trial of Neuraltus’ NP001 is anticipated. And, phase II go/no go decisions could be made on emerging therapies for ALS including GlaxoSmithKline’s ozanezumab and the generic mexiletine as early as the end of the 2014.
Riluzole, however, remains the only FDA-approved drug to slow progression of the disease – extending survival by about 3 – 6 months.
Although a more effective treatment for ALS remains currently elusive, an increasing number of interventions are becoming available to people with ALS that can improve survival and quality of life.
Exercise improves outlook and well-being. Nutrition plans and breathing devices may extend survival according to multiple studies. And, a growing number of medicines are becoming increasingly available to help relieve key symptoms of ALS including emotionality, muscle pain, stiffness and spasticity.
But despite the increased therapeutic options available to people with ALS, according to California Pacific Medical Center’s Robert Miller MD “these treatments remain underutilized.”
This month, ALS experts gathered at the 2014 meeting of the American Academy of Neurology (AAN 2014) in Philadelphia to discuss therapies for today's people with ALS. And, how to improve the care of people with ALS going forward.
Symptoms Check
Most symptoms of ALS can be treated says Miller.
Nuedexta, FDA approved for use in 2010, reduces emotionality (pseudobulbar affect) by 50% according to studies led by Carolinas Medical Center Benjamin Brooks MD. But although these symptoms may occur in as many as 1 out of 2 people with ALS, only about 50% by some estimates are treated for the condition.
Freeze frame? Botox is emerging as a potential second-line treatment to reduce saliva production (sialorrhoea) in people with ALS that do not respond to existing medications. However, the procedure must be delivered by an experienced healthcare professional trained in the procedure according to neurologist Pierre-Francois Pradat MD. And, cautions Pradat, in rare instances the toxin has been reported to spread to nearby muscles needed to chew and swallow foods - exacerbating the disease.
The reason, according to a 2014 AAN analysis, led by Brooks and Miller, is that some physicians appear to be unfamiliar with pseudobulbar affect. And/or are unaware of medicines now available to treat these symptoms.
The condition, according to a 2013 analysis by Pennsylvania State University neurologist Zachary Simmons MD, may also be confused with other psychiatric illnesses including bipolar disorder and clinical depression, due to increased avoidance, fear and social isolation which can result due its disruptive and embarrassing nature.
Sialorrhoea (excess saliva) is becoming more manageable. As many as 2 out of 3 people with ALS appear to benefit from existing medications by some estimates. But as few as 1 out of 5 people with ALS receive them according to a 2014 AAN analysis.
What’s more, according to Hôpital de la Pitié-Salpétrière’s Pierre-Francois Pradat MD, radiation therapy is increasingly successful in managing these symptoms in people with ALS who do not respond to these medicines – a treatment being increasingly used in France. And, beginning to be used elsewhere in Europe.
The radiotherapy, developed in collaboration with radiation oncologist Avi Assouline MD, takes advantage of a key downside of radiotherapy for head and neck cancers: dry mouth. The procedure, however, uses much lower doses of radiation to reduce saliva production - to minimize side effects.
The strategy, according to a 2014 study of 50 people with ALS, appears to be safe, well tolerated and reduced salivation to near normal levels (Sialorrhoea Score Scale 1-3) in more than 90% of those treated.
“Many of our patients that did not respond to existing medications felt isolated and depressed. But after treatment, their social lives began to return to normal.” says Pradat. “Radiotherapy really can improve the life of some people with ALS.”
Management Sciences
While pseudobulbar affect and sialorrhoea are undertreated, according to the 2014 AAN report, the management of these symptoms is steadily increasing due at least in part to revised 2009 AAN and 2012 EFNS ALS practice guidelines. Other strategies, however, says Miller, remain staunchly underutilized.

Weigh station Some people with ALS may need a feeding tube to maintain their weight. But clinicians remain divided on how or when to do the procedure. And, no evidence-based practice guidelines are in place. Image: Paola Kizette Cimenti, Flickr.
Maintaining weight can extend life by an average of 9 months according to studies led by Hôpital Dupuytren nutrition specialist Jean-Claude Desport MD in Limoges. But as many as 1 out of 2 people with ALS are undernourished. And, less than 1 out of 2 people with ALS by some estimates recommended to use a feeding tube elect not to do so.
“I would really encourage patients to treat their weight as something they could do medically to improve their survival," says Massachusetts General Hospital neurologist Anne-Marie Wills MD MPH. "And, to accept a feeding tube earlier in their disease."
Furthermore, less than 1 out of 5 people with breathing difficulties by some estimates use non-invasive ventilation such as a BiPAP machine – a treatment strategy that according to a growing number of studies extends life to an average of 5 years.
In hopes to deliver better care to more people with ALS, a team of 10 neurologists led by CPMC’s Robert Miller MD and Carolinas Medical Center’s Benjamin Brooks MD implemented a series of measures to evaluate existing care for people with ALS. And, identify clear gaps that need to be filled.
“When you start to measure quality of life, it begins to improve,” says Miller.

Breathe easier? The NeuRx diaphragm pacing system may help improve breathing by increasing the stamina of diaphragm muscles. But unlike non-invasive ventilation, clinicians remain divided on whether the device improves quality of life and increases survival of people with ALS. Clinical trials are ongoing. Image: Synapse Biomedical.
Rethinking cognition in ALS
But the increased use of therapeutic options is not the only aspect of care for people with ALS that needs a boost according to a 2014 AAN analysis.
As many as 1 out of 2 people with ALS may experience cognitive challenges according to studies led by Trinity College School of Medicine’s Orla Hardiman MD. People who appear to progress more quickly. And, experience breathing difficulties more rapidly and loss of muscle strength.
Nevertheless, no standardized guidelines are in place to diagnose people with cognitive challenges. And, which test to use to identify these deficits remains hotly debated.
These challenges include deficits in executive function - difficulties in planning, organizing, time management and making decisions.
“Families want to know what they are up against,” says Miller.
A number of tests are available to spot cognitive challenges in people with neurological conditions. The problem according to University of Pennsylvania School of Medicine neurologist and neuropsychologist Murray Grossman MD EdD is that the results are often confounded by challenges inherent to the disease itself.
Many of these tests can be physically exhausting. And the tasks are often timed – a challenge for people with ALS with executive deficits.
New tests may need to be designed for people with ALS – taking into account these challenges.
“We do not want to exhaust our patients,” explains Grossman. “The idea is to create a test that is most sensitive [to these changes] that can be done in the shortest amount of time.”
Testing 1,2,3 The ECAS is a short 15 minute test that helps clinicians spot challenges that could be experienced by people with ALS including critical thinking, producing words and interpreting emotions. Image: ECAS, Sharon Abrahams PhD, University of Edinburgh.
The Edinburgh Cognitive Assessment Screen (ECAS) is emerging as a promising tool to identify the first signs of cognitive challenges in people with ALS.
The ECAS, developed by University of Edinburgh neuropsychologist Sharon Abrahams PhD, aims to identify a broad range of behavioral and cognitive challenges experienced by people with ALS - including expressing thoughts, interpreting emotions and producing words.
Existing tests for people with ALS, including the ALS Cognitive Behavioral Screen (ALS-CBS) used frequently in US clinics, focus on only some of these challenges.
The ECAS appears to be easier for people with ALS to do according to a study of 80 people with ALS led by Grossman.
Most people with ALS completed the ECAS regardless of physical abilities according to results presented by University of Pennsylvania’s School of Medicine’s Eileen Moran BS MSc at AAN 2014. In contrast, only about 1 out of 2 people were able to complete the Philadelphia Brief Assessment of Cognition (PBAC).
The PBAC is increasingly being used to identify key cognitive challenges in a broad range of neurodegenerative diseases including Alzheimer’s disease and frontotemporal dementia (FTD).
The ECAS is currently being evaluated in a growing number of clinics in the US and Europe.
“It is important to have an international view of ALS. And see if it differs in other parts of the world,” says Grossman.
To learn more about cognition and ALS, check out Cognition in ALS: Measure for Measure. To find out about emerging compensatory mechanisms that may help many people with ALS retain key cognitive abilities, check out Rethinking ALS.
Pain, is it any wonder?
Pain continues to be underestimated, underreported and undertreated in people with ALS according to experts at AAN 2014.
Nearly 40% of people with ALS experience moderate or severe pain according to a retrospective analysis of electronic medical records of nearly 1200 people with ALS led by Pennsylvania State University neurologist Zachary Simmons MD.

Trials on tv? Mexiletine is one of a growing number of strategies being tested with the help of telemedicine. The approach, first deployed to provide care for soldiers overseas, aims to expedite development of therapeutic options by reducing clinic visits. "The faster we enroll our studies and the better we retain our patients in them, the faster we will develop better treatments. And, the faster we will get to a cure," says Duke University neurologist Richard Bedlack MD PhD. Image: Kevin Downey, Tripler Army Medical Center, Hawaii.
But pain could occur in as many as 2 out of every 3 cases of ALS according to a study of 100 people with ALS in France presented at AAN 2014 by Centre Hospitalier Universitaire de Clermont-Ferrand’s Natalie Guy-Renouil MD.
Pain appears to occur in people with both bulbar and limb onset ALS according to a growing number of studies. And, according to Guy-Renouil, its severity does not appear to correlate with the progression rate of the disease.
Standardized guidelines to manage pain in people with ALS remain lacking. But mexiletine is emerging as a potential treatment for muscle cramps, a key source of pain experienced by people with ALS, particularly early in their disease.
Mexiletine is currently being used to reduce muscle stiffness in people with a growing number of muscle diseases known as non-dystrophic myotonias.
A phase IV trial, led by University of California Davis neuromuscular disease specialist Bjorn Oskarsson MD, is underway in Sacramento. Trial sites include the University of California Davis Medical Center. And, all registered telemedicine centers in California according to Oskarsson.
A phase II clinical trial of mexiletine, led by University of Washington School of Medicine’s Michael Weiss MD, is also ongoing.
The first results are expected by the end of the 2014.
To learn more about pain and ALS, check out Taming the Charley Horse in ALS. To learn more about mexiletine, check out Mexiletine, channeling ALS?
Exercise does a body good?
Range of motion and stretching exercises help keep muscles and joints loose. And, reduce muscle stiffness and muscle pain. But staying active according to a growing number of studies may do much more for people with ALS.
Emerging aerobic workouts including stationary cycling and treadmilling may help keep motor neurons healthy by boosting energy supplies, sweeping out potentially toxic aggregates, reducing inflammation, and turning up production of nutritious substances known as neurotrophins.

Exercise does a body good? Certain exercises appear to be safe for people with ALS. But how much exercise remains an open question. Image: LuluLemon Athletica, Flickr.
“In ALS, we need to keep people with ALS moving to avoid deconditioning,” says Carolinas Medical Center exercise physiologist and physical therapist Mohammed Sanjak PhD PT MBA. “Reduce the loss of flexibility and muscle strength.”
Certain workouts including stationary cycling appear to be safe according to preliminary results from a study led by Johns Hopkins University School of Medicine’s Nicholas Maragakis MD. But these exercise routines, according to Sanjak who is participating in the study, must be tailored for each person with ALS.
“It is like medicine,” says Sanjak. “It needs to be personalized.”
To help clinicians create exercise routines for people with ALS, Sanjak turned to the Veterans Specific Activity Questionnaire (VSAQ), a short Q & A that estimates exercise abilities.
The questionnaire, introduced by Stanford University School of Medicine’s Victor Froelicher MD, is commonly used to estimate exercise tolerance in people battling heart disease and/or at high risk of developing heart failure.
Exercise capacity, estimated by the VSAQ, appears to correlate well with the ALS revised functional rating scale (ALSFRS-R) motor subscore (p < 0.001) – a frequently used measure of key functional abilities in people with ALS including walking and climbing stairs according to recent results presented by Sanjak at AAN2014
What’s more, the VSAQ, appeared to perform well (p < 0.001) in estimating the amount of exercise people with ALS could do – including in frequently used exercise tests such as the 6 minute walk (6MWT) and time up and go (TUG).
77 people with ALS participated to date. The study remains ongoing.
To learn more about exercise, check out Exercise: stretching the limits of ALS care.
To do list

Unraveling ALS? With the advent of next-generation sequencing methods, more than 30 genes may be linked to ALS according to the University of Massachusetts Medical Center's Robert Brown MD PhD. Image: Roy Kaltschmidt for Lawrence Berkeley National Labs, Flickr.
There is a lot more work however that needs to be done according to CPMC’s Robert Miller MD.
More people with ALS need to be referred to multidisciplinary care centers – where possible. And, palliative care plans need to be put in place.
With the discovery of a link between C9orf72 and ALS, the re-definition of familial ALS is also desperately needed according to recent studies led by Kings College London’s Ammar Al-Chalabi MD and Trinity College of Medicine’s Orla Hardiman MD. And, guidelines for genetic testing according to Miller need to be developed.
ALS is becoming increasingly clear to be “a syndrome” says University of California San Francisco’s Jeffrey Rosenfeld MD PhD. A disease which is on a clinical spectrum that spans ALS, primary lateral sclerosis (PLS), primary muscular atrophy (PMA) and frontotemporal dementia (FTD).
And, ALS is extremely heterogenous. According to University of Massachusetts Medical Center’s Robert Brown MD PhD, more than 30 genes may be linked to the disease.
“The issue of genetic testing is becoming increasingly important,” says Miller. “Who to test? When to test? This is in evolution. It is one of the areas we need to focus on.”