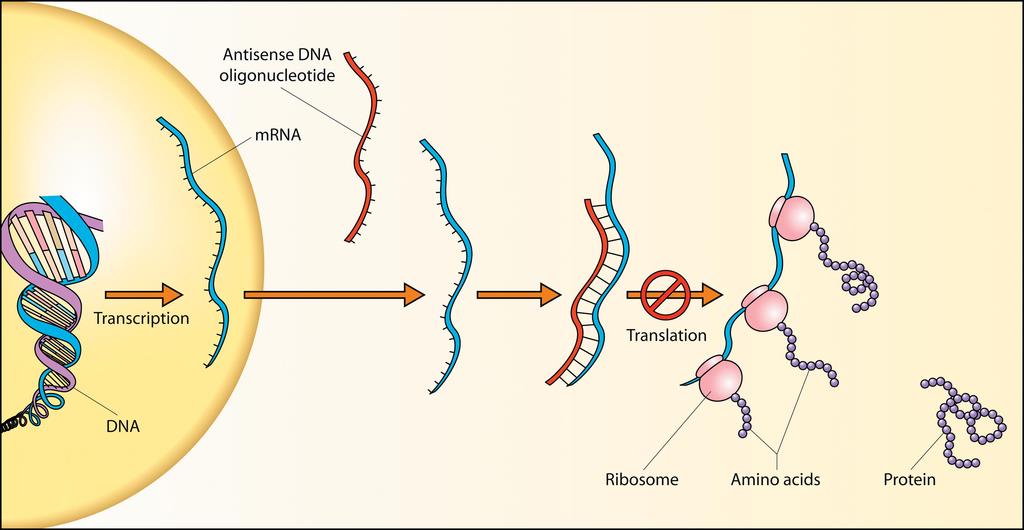
Diagram of an ASO. By Robinson R./Wikimedia Commons
Antisense Oligonucleotides, or ASOs, are small single-stranded molecules of DNA with a great deal of potential to help patients with genetic disorders like ALS, commonly known as Lou Gehrig’s disease. However, to better understand how to effectively use them, we will need to better understand the mechanisms by which ALS damages human cells – a big part of our research at the ALS Therapy Development Institute (ALS TDI).
How ASOs Work
ASOs are easily absorbed by cells, where they attach themselves to “messenger” mRNA strands. They can then, in effect, “turn down” a gene, disrupting the cell’s natural production of a particular protein. This is useful in treating genetic conditions, where mutations in our DNA can cause cells to produce harmful proteins or prevent them from producing those that our body needs to function.
Gain vs. Loss of Function Mutations
However, ALS is a complex neurodegenerative disease. Research shows it can be caused by a number of different mutations, varying from case to case, and not all genetic mutations work in the same way. In the case of ASOs, they appear to be particularly effective in treating “gain-of-function” mutations, as opposed to “loss-of-function” mutations.The key difference between these two types of mutations is how they affect the proteins that a cell produces. A gain-of-function mutation causes a cell to produce a protein that does something it’s not supposed to do, which is often toxic to the body. On the other hand, a loss-of-function mutation causes the production of a protein that is unable to carry out its necessary functions. Both can have a damaging impact, but in different ways. Also, the two scenarios are not mutually exclusive.
ASOs, because they work by preventing a cell from making a specific protein, have shown promise for treating gain-of-function mutations. They can target cells that are producing toxic proteins and stop them. However, because they work by turning a cell’s protein production “off,” their potential to treat loss-of-function mutations is limited. ASOs can reduce or eliminate a protein we don’t want, but they generally can’t bring back or fix a protein that isn’t fulfilling its function, with some exceptions.
ASOs and ALS
There is no conclusive evidence that ALS is primarily caused by one type of mutation or the other – it’s likely a combination of the two. However, there are common mutations in ALS, like that of the SOD1 gene, that are believed to be gain-of-function mutations. In early 2023 the FDA approved called Qalsody, also known as tofersen, for treating SOD1 ALS. This represents the first, and currently only, ASO treatment approved for any form of ALS.
“ASOs are really promising,” says ALS TDI CEO and Chief Scientific Officer Fernando Vieira, M.D. “But that doesn't mean that it's going to be a one-size-fits-all solution for every genetic mutation in ALS.”
While ASOs have more potential for gain-of-function mutations, other treatments, including viral gene therapy and small molecule compounds, could possibly treat loss-of-function mutations. Combining therapies targeting each type of mutation could be a strategy for future approaches to ALS treatment. There may also be potential for the future development of ASOs that are able to target loss-of-function mutations. This approach has been explored in other diseases, such as Spinal Muscular Atrophy (SMA). Spinraza, the first FDA-approved drug for SMA, is an ASO that targets a loss-of-function mutation in the SMN2 gene.
Moving forward, researchers will continue to explore the effectiveness of the ASOs currently in clinical trials. “And In the meantime, we at ALS TDI and others are spending some of our resources trying to better understand how each of these mutations can actually cause cell death,” says Dr. Vieira. “If we have a better sense of which mutations are loss-of-function and which are gain-of-function, we'll definitely have more guidance on which strategies to take into the clinic.”
What to do Next: