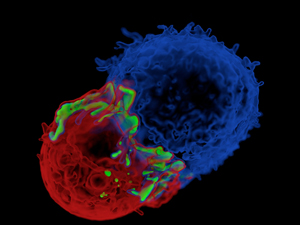
Par-foxP3? Regulatory T cells (red) may help protect motor neurons in people with ALS in part by reducing the production of inflammatory substances by key immune cells (blue) including effector T cells that infilitrate the CNS. Image: John R James PhD and Ron Vale PhD. Courtesy of Howard Hughes Medical Institute. All rights reserved.
About 1 out of 10 people with ALS live at least 5 to 10 years. But many more survive only 2 to 3 years after being diagnosed with their disease.
Researchers are working hard to understand why certain people with ALS live longer in hopes to design therapies to help fight the disease.
One emerging competitive advantage against ALS is a high number of regulatory T cells, key immune cells that may help protect motor neurons by keeping inflammation in check.
People with ALS who live at least 6 years after diagnosis appear to have three times the number of regulatory T cells in circulation compared to those that progress much more rapidly according to a 2013 analysis led by Houston Methodist Hospital neurologist Stanley Appel MD.
What’s more, the larger the number of these immune cells that are on ‘the course’ in people with ALS, the slower the progression of their disease.
“The number of regulatory T cells seem to correlate with doing better,” explains Appel.
The results suggest that increasing populations of regulatory T cells may help more people with ALS be on their 'A' game. But how to boost the number of these cells in people with ALS remains unclear.
A growing group of clinicians in France suspect that low dose interleukin 2 (IL-2) may help expand regulatory T cell populations in people with ALS. And, thereby slow the progression of their disease.
“If there is a real causative effect between the number of T regulatory cells and survival, then the margin for benefit is quite wide,” explains Assistance Publique – Hôpitaux de Paris clinical pharmacologist Gilbert Bensimon MD PhD, leader of the study. “It is much larger than what we achieved with riluzole.”
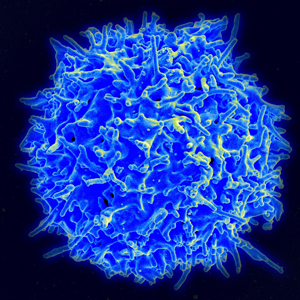
Bump and run? The surface of regulatory T cells are highly decorated with high affinity receptors that tightly bind IL-2 - enabling them to be potentially selectively expanded by lose doses of IL-2. Image: NIAID.
The treatment strategy, originally developed to fight transplant rejection, is one of the first potential ALS treatments to be tested in the clinic that aims to boost regulatory T cell populations in people with the disease.
A phase I/II clinical trial is scheduled to begin in the fall of 2014.
Therapy to a T?
In the mid 2000s, Dana Farber Cancer Institute’s Jerome Ritz MD turned to IL-2 in hopes to promote tolerance in stem cell transplant recipients at high risk of developing grafts versus hosts disease (GVHD).
The growth substance, at low doses, according to studies led by Ritz, appears to stimulate the proliferation of regulatory T cells. But leave troublesome effector T cells, lacking high affinity IL-2 receptors, untouched.
The approach is emerging as a potential strategy to treat a growing number of autoimmune diseases. And, reduce the risk of transplant rejection.
“The objective,” explains Gilbert Bensimon MD PhD, “is to control untoward immune responses by re-establishing the physiological balance of regulatory T cells and effector T cells in the immune system.”
The treatment strategy, according to a growing number of phase I and phase II clinical studies, appears to double numbers of circulating regulatory T cells - at least in people at high risk of GVHD. And, boost levels of FOXP3 – a key regulatory substance critical to help these cells keep inflammation in check.
Low-dose IL-2 therapy is being developed in the US to help fight transplant rejection in people with certain blood diseases.
The approach is also being evaluated by Hôpital Pitié-Salpêtrière immunologist David Klatzmann MD PhD in France as a potential treatment for type I diabetes and complications of certain viral infections.
A chip shot? Low dose IL-2 therapy aims to restore order in the immune system in people with ALS by re-establishing the balance of regulatory T cell and effector T cell populations.
Now, Gilbert Bensimon MD PhD is gearing up to put low dose IL-2 to the test in people with ALS in hopes to increase numbers of regulatory T cells and thereby slow progression of their disease.
A phase I/II randomized placebo-controlled clinical trial is to take place in France. Participating sites include Centre Hospitalier Régional Universitaire de Nîmes and Centre Hospitalier Régional Universitaire de Montpellier. 24 people with ALS are expected to participate.
The 6 month study aims to evaluate the safety and tolerability of low doses of IL-2 in people with ALS. And, determine the ability of the drug to increase the regulatory T cell count in people with the disease.
The results are also expected to help clinicians identify the optimal dose to target the ‘sweet spot’ in people with ALS to expand these immune cells. A regimen that might differ in people with other disease indications.
“We really need to know what dose can effectively upregulate regulatory T cells [alone]. And, make sure the safety margin is the same," says Stanley Appel MD, who is not participating in the study.
The first results are expected sometime in 2015.
***
To find out more about the potential of IL-2 for people with ALS, tune into our Postcard from France, T regulator. To learn more about the role of regulatory T cells in ALS, check out Regulating ALS.
Patient Resources
Immunomodulation in ALS (IMODALS): A phase I/II of safety and activity of low dose interleukin in ALS. Contact | ALS TDI | Website
References
Kennedy-Nasser, A. et al. (2014) Ultra low-dose IL-2 for graft-versus-host disease prophylaxis after allogeneic HSCT mediates expansion of regulatory T cells without diminishing anti-viral and anti-leukemic Activity. Clinical Cancer Research doi:10.1158/1078-0432.CCR-13-3205 Abstract | Full Text (Subscription Required)
Matsuoka, K. et al. (2013) Low-dose interleukin-2 therapy restores regulatory T cell homeostasis in patients with chronic graft-versus-host disease. Science Translational Medicine 5(179), 179ra43. Abstract | Full Text (Subscription Required)
Henkel, J.S, Beers, D.R., Wen, S., Rivera, A.L., Toennis, K.M., Appel, JE, Zhao, W., Moore, D.H., Powell, S.Z. and Appel, S.H. (2013) Regulatory T-lymphocytes mediate amyotrophic lateral sclerosis progression and survival. EMBO Molecular Medicine 5(1), 64-79. Abstract | Full Text
Beers, D.R., Henkel, J.S., Zhao, W., Wang, J., Huang, A., Wen, S., Liao, B. and Appel, S.H. (2011) Endogenous regulatory T lymphocytes ameliorate amyotrophic lateral sclerosis in mice and correlate with disease progression in patients with amyotrophic lateral sclerosis. Brain 134(5), 1293-1314. Abstract | Full Text
Saadoun, D., Rosenzwajg, M., Joly, F., Six, A., Carrat, F., Thibault, V., Sene, D., Cacoub, P. and Klatzmann, D. New England Journal of Medicine 365(22), 2067-2077. Abstract Full Text
Koreth, J. et al. (2011) Interleukin-2 and regulatory T cells in graft-versus-host disease. New England Journal of Medicine 365(22), 2055-2066. Abstract | Full Text
Zorn, E. et al. (2006) IL-2 regulates FOXP3 expression in human CD4+CD25+ regulatory T cells through a STAT-dependent mechanism and induces the expansion of these cells in vivo. Blood 108(5), 1571-1579. Abstract | Full Text
Further Reading
Bluestone, J.A. (2011) The yin and yang of interleukin-2-mediated immunotherapy. New England Journal of Medicine 365(22), 2129-2131. Abstract | Full Text (Subscription Required)
Note:An earlier version of this article appeared in March 2014. The story has since been revised and updated.