 The second day of the International ALS/MND Research Symposium started off with a talk from Kevin Eggan of Harvard University (pictured). For many, Dr. Eggan is recognized as the first person to create an induced pluripotent stem cell line from a person diagnosed with ALS (the technology and process to create iPS cells was invented previously by Shinya Yamanaka, M.D., Ph.D. of Kyoto University in 2006). Dr. Eggan’s talk dove deep into asking whether or not these type of stem cells were living up to their potential as drug development tools, and he provided some interesting results from his analysis of the field to date.
The second day of the International ALS/MND Research Symposium started off with a talk from Kevin Eggan of Harvard University (pictured). For many, Dr. Eggan is recognized as the first person to create an induced pluripotent stem cell line from a person diagnosed with ALS (the technology and process to create iPS cells was invented previously by Shinya Yamanaka, M.D., Ph.D. of Kyoto University in 2006). Dr. Eggan’s talk dove deep into asking whether or not these type of stem cells were living up to their potential as drug development tools, and he provided some interesting results from his analysis of the field to date.
According to Dr. Eggan, his lab can coax mature adult fibroblasts to revert to a state of pluripotency using the Yamanaka factors, inserting into the nucleus of those cells several genes which induce their revision into stem cells. One of the challenges with this method is that these genes randomly insert themselves into the genome of the cell and remain there in perpetuity. However, the cells do become stem cell like. Newer methods to induce to revert to a stem cell state are being used by other labs, including ALS TDI, which don’t rely on random gene insertion approach. Regardless, the Eggan lab differentiated its iPS cells into motor neurons over a period of 24 days on average, creating a disease-relevant cell line to study. Before subjecting this cell line to experiments, the team spends about 30 days confirming its status and stability.
Of interest to the Eggan lab was to look at whether or not there were differences in the way electrical currents traveled across the ALS motor neurons. They used sophisticated technology to shoot a current across several different lines created from PALS with different ALS-associated gene mutations, including SOD1. Interestingly, they found that the SOD1 A4V lines had the greatest number of action potential spikes (a way to measure the amount/speed at which neurons communicate with surrounding cells, such as other neurons or astrocytes) of all the lines they looked at, suggesting that perhaps different forms of familial ALS may have specific cellular phenotypes, which could help explain the different trajectories of disease and be used in drug development experiments.
 Speaking of drug development, the Eggan Lab earlier in 2014 announced that it had taken this information on action potential and begun to screen potential drugs which may modify its expression or amplification back to what is seen in non-ALS cell lines. One such drug screened, retigabine, showed the greatest benefit in the lab’s cell based screen.
Speaking of drug development, the Eggan Lab earlier in 2014 announced that it had taken this information on action potential and begun to screen potential drugs which may modify its expression or amplification back to what is seen in non-ALS cell lines. One such drug screened, retigabine, showed the greatest benefit in the lab’s cell based screen.
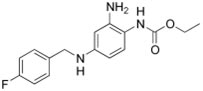
Retigabine (pictured) is thought to open potassium acid channels and correct the sodium channel regulation in motor neurons. It is an FDA approved compound for the treatment of certain forms of epilepsy and, together with the Northeast ALS Consortium, a 120 person clinical trial is being planned at 12 NEALS sites. Enrolled participants will have the opportunity to be placed into either the treatment group (which will include two different dosing groups) or a placebo control group. No date was given for when patient screenings will begin, site locations, or when exclusion criteria will be available for this trial. When the trial does begin, it will be the first trial to be launched on the basis of information gathered from iPS lines only in ALS. It is not known whether iPS cell lines are “better” tools for drug screening than more common models including fruit flies, mice, and other animals. However, this trial will provide an opportunity to begin to answer that question for the first time, at least in ALS research.
 There were several other speakers during this first session of the day which focused on in vitro modeling. Two such talks were given regarding the characterization of iPS cells created from C9orf72 patient samples. Roxanne Mutihac, Ph.D. of the Nuffield Department of Clinical Neurosciences at the University of Oxford (pictured), provided data from her research on two C9orf72 iPSc lines she created. In one of her lines, she reported that it maintained a total of 1380 hexanucleotide repeats and in the other, 510 were maintained through the reprogramming process. After confirming that the expansion was stable, she began studying the cells and found a key hallmark of C9orf72 pathology- the presence of toxic RNA foci within the cells. Other interesting findings reported included the phenomenon of high levels of calcium in C9orf72 motor neurons versus cortical neurons, which may suggest a unique trait for further study. Finally, it is worth noting that in the age of oligogenetics in ALS, TDP43 proteins mislocalized in the C9orf72 iPSc lines created in Mutihac’s lab.
There were several other speakers during this first session of the day which focused on in vitro modeling. Two such talks were given regarding the characterization of iPS cells created from C9orf72 patient samples. Roxanne Mutihac, Ph.D. of the Nuffield Department of Clinical Neurosciences at the University of Oxford (pictured), provided data from her research on two C9orf72 iPSc lines she created. In one of her lines, she reported that it maintained a total of 1380 hexanucleotide repeats and in the other, 510 were maintained through the reprogramming process. After confirming that the expansion was stable, she began studying the cells and found a key hallmark of C9orf72 pathology- the presence of toxic RNA foci within the cells. Other interesting findings reported included the phenomenon of high levels of calcium in C9orf72 motor neurons versus cortical neurons, which may suggest a unique trait for further study. Finally, it is worth noting that in the age of oligogenetics in ALS, TDP43 proteins mislocalized in the C9orf72 iPSc lines created in Mutihac’s lab.
ALS in China, the US Military and Head Injury
An entire session at this year’s International Symposium was devoted to the epidemiology of ALS. It included important reports on the landscape of ALS in China, new data on military incidence of ALS from the US, and a conversation on whether head injuries (ie: concussions) alter the progression of ALS.
China is the world’s most populous country with more than 1.3 billion people. It is an immensely diverse demographic, and results reported at this year’s meeting from Liying Cui, Ph.D. of the Peking Union Medical College in Beijing, suggest that the population of PALS in China may be very different from that found in other nations across the globe. According to Cui, 95% of ALS cases in China are sporadic, and the ALS-associated genes found in Chinese PALS are very different from those found in western countries. However, there are some similar characteristics. The mean age of onset of ALS in China is about 52 years of age in PALS, and the time from symptom onset to diagnosis is generally about 13 months- statistics not wholly unlike what we see in many other countries.
Recently, Cui and her colleagues in 10 different research hospitals created an ALS registry, recruiting and documenting 461 PALS from across China. According to China ALS Registry data, only 29% of PALS take rilutek versus 39% which opt for traditional herbs to treat the disease. In a separate study of 680 PALS, Cui reported on the site of onset and spread of disease in Chinese PALS. More than half of all PALS in the study were found to have their first symptoms in upper limbs generally (cervical), with another 1 in 5 cases experiencing the first symptoms in either bulbar or lumbar regions. According to this new study, 85% of PALS developed symptoms in the upper and lower motor neurons, with 10% lower motor neuron only. The mean survival of PALS in this study was 34 months with bulbar onset ALS (PALS survive only 12 months on average in China). As seen and reported in other epidemiological studies of ALS, Cui suggested that the data confirmed that the number of regions of the spinal cord involved in the first three months of disease onset seem to correlate with the overall pace of the disease.
For many years, ALS was not thought to be related to dementia. However, more recent studies have now shown different cognitive and executive dysfunctions in PALS. In the US, it is now thought that at least 10% of PALS develop frontotemporal dementia in addition to the progressive neurodegenerative disease. However, according to Cui’s research, the percentage of ALS/FTD in China is only 2% overall. Similarly, it seems ALS-associated genes in China vary greatly from those found in western nations. Less than 1% of FALS cases in China are carriers of the C9orf72 expansion, according to Cui. More commonly found are SOD1 (26%), TDP43 (5.6%), and FUS (12%).
 It is a commonly cited fact in the US that deployed military service members have a greater chance of developing ALS than the civilian population. However, little additional data has been reported since the original work was presented more than a decade ago. Marc Weisskopf, PhD, ScD (pictured) of the School of Public Health at Harvard University provided his analysis of the National Longitudinal Mortality Study, a sampling of households within the US. In this data, he identified 800 ALS deaths, including 221 military service members through 2002. Nearly two thirds of these PALS served in the Second World War (WWII), with the others serving in the Korean, Vietnam, or other wars except World War I. Weisskopf’s review of the Mortality Study found there were different rates of ALS within the military over time, with WWII veterans developing ALS at a great rate when compared to veterans from Korea or Vietnam. He suggests there may be other deployment-related linkages which need to be explored.
It is a commonly cited fact in the US that deployed military service members have a greater chance of developing ALS than the civilian population. However, little additional data has been reported since the original work was presented more than a decade ago. Marc Weisskopf, PhD, ScD (pictured) of the School of Public Health at Harvard University provided his analysis of the National Longitudinal Mortality Study, a sampling of households within the US. In this data, he identified 800 ALS deaths, including 221 military service members through 2002. Nearly two thirds of these PALS served in the Second World War (WWII), with the others serving in the Korean, Vietnam, or other wars except World War I. Weisskopf’s review of the Mortality Study found there were different rates of ALS within the military over time, with WWII veterans developing ALS at a great rate when compared to veterans from Korea or Vietnam. He suggests there may be other deployment-related linkages which need to be explored.
Before moving on to head injury and ALS, it is worth noting an important talk from Daniela Mariosa, a Ph.D. student at the Karolinska Institute in Stockholm, Sweden. Mariosa’s research concerned diabetes as a risk factor in the development of ALS, which was originally suggested in a paper from Martin Turner, M.D., Ph.D. last year. Mariosa decided to look at the 1990 Swedish census, in which she identified 5108 newly diagnosed ALS cases. Controlling nearly 5:1 with non-ALS cases in the census, Mariosa found that an insulin-dependent diabetes diagnosis before age 30 increased the likelihood of developing ALS.
 There has been great attention paid to the topic of head injury in the US as of late, with the National Football League (NFL) recently settling a class-action lawsuit of former players claiming the injuries they suffered while playing caused them to develop several different neurodegenerative diseases, including ALS. An original research study done by Everett Lehman at the National Institute of Occupational Safety and Health found a greater incidence rate of neurodegeneration in former NFL players as compared to the general population, a summary of which was provided via webinar by the ALS Therapy Development Institute in 2012. Notable former NFL players diagnosed with ALS include Philadelphia Eagles fullback Kevin Turner (Kevin Turner Foundation), New Orleans Saint’s hero Stephen Gleason (Team Gleason) and journey-man linebacker Tim Shaw (pictured, @TShawsTruth). Despite the evidence of some kind of correlation between ALS and the NFL, Lehman and most others have been careful to clearly state their studies are not intended to measure if concussions or other type of injuries play a direct role in ALS onset.
There has been great attention paid to the topic of head injury in the US as of late, with the National Football League (NFL) recently settling a class-action lawsuit of former players claiming the injuries they suffered while playing caused them to develop several different neurodegenerative diseases, including ALS. An original research study done by Everett Lehman at the National Institute of Occupational Safety and Health found a greater incidence rate of neurodegeneration in former NFL players as compared to the general population, a summary of which was provided via webinar by the ALS Therapy Development Institute in 2012. Notable former NFL players diagnosed with ALS include Philadelphia Eagles fullback Kevin Turner (Kevin Turner Foundation), New Orleans Saint’s hero Stephen Gleason (Team Gleason) and journey-man linebacker Tim Shaw (pictured, @TShawsTruth). Despite the evidence of some kind of correlation between ALS and the NFL, Lehman and most others have been careful to clearly state their studies are not intended to measure if concussions or other type of injuries play a direct role in ALS onset.
Instead, the goal of their studies was to explore if head injuries affect the progression rate of the disease. Christina Fournier, M.D., an instructor at Emory University, reported on her research into this question. She presented data suggesting no correlation between a head injury (which she defined as causing the loss of consciousness or hospitalization) and the progression rate of ALS. Using data from Emory University, she found 24 PALS which met her criteria for head injury and compared them to 76 cases which didn’t. Fournier also looked at autopsy samples from PALS with and without head injury, and found no major differences in the frequency of proteinopathies in TDP-43, Tau, and others. In summary, more research is needed before a definitive connection between head injury and ALS can be identified.
Neurofilaments as ALS Biomarker
One of the greatest challenges in ALS drug development is the lack of biomarkers to predict disease progression. Biomarkers are typically defined as a measureable indicator of the presence or severity of a disease in patients. Most of the time, ALS progression is measured using a patient-reported and rather subjective scale known as the revised ALS Function Rating Scale, a questionnaire used by clinicians to note changes in a PALS’ ability to move, eat, or breathe independently. Earlier in 2014, the ALS Therapy Development Institute called together more than 30 scientists for a biomarker research meeting, co-hosted with The ALS Association and NINDS, to discuss the latest data- some of which was later presented at the International Symposium in December.
 According to Robert Bowser, Ph.D. (pictured), one of the foremost leaders in biomarker research in ALS, there is a huge gap between the discovery and validation of biomarkers. A review of the published work in this field conducted by Bowser showed there have been more than 20,000 publications on potential biomarkers in neurodegenerative disorders such as ALS. However, only 318 of those publications specifically aimed to validate a proposed biomarker. This important gap highlights the difference between basic, observational research and the application of those observations in a drug development or clinical setting.
According to Robert Bowser, Ph.D. (pictured), one of the foremost leaders in biomarker research in ALS, there is a huge gap between the discovery and validation of biomarkers. A review of the published work in this field conducted by Bowser showed there have been more than 20,000 publications on potential biomarkers in neurodegenerative disorders such as ALS. However, only 318 of those publications specifically aimed to validate a proposed biomarker. This important gap highlights the difference between basic, observational research and the application of those observations in a drug development or clinical setting.
At this year’s International Symposium, a special session on biomarkers focused on the changes in the presence of neurofilaments in PALS overtime as a valid biomarker of disease progression. Filaments play a major role in the structural health of cells, and a specific class of them known as neurofilaments can be found in motor neurons. As any cell degenerates, its shape, size, and overall structure (cytoskeleton) changes. Neurofilaments have been looked at in ALS as a potential way to measure the overall health of motor neurons for many years; however since they are primarily found in cells within the spinal cord, assessing neurofilament levels is both costly and difficult.
Two of the presenters during the biomarker session speaking on neurofilaments in ALS, Martin Turner, Ph.D. of Oxford and Andrea Malaspina, M.D., Ph.D., decided to skip protocol and to present back-to-back and then to take questions together from the audience. Similar in topic, the data they would be presenting resulted from a collaborative effort on their parts.
Malaspina began with an overview of neurofilaments and review of previous research. Neurofilament auto-antibodies increase as ALS progresses and the neurons degenerate. However, there are many different forms of neurofilament chains. Typically, they are separated based on weight into three different categories or subunits: light, medium, and heavy. The loss of neurofilaments is not unique to ALS, and decreases have been associated with all sorts of disorders of the spinal cord which are associated with degeneration or damage to motor neurons, including spinal cord injuries. According to Malaspina’s research, ALS stands out- at least when it comes to the light subunit of neurofilament (NfL). In his research on plasma and cerebrospinal fluid (CSF) samples, he discovered a correlation between the increase and decrease in the level of NfL present. This may be an important finding as blood samples are easier to collect and analyze than CSF; both for the patient as well as the researcher.
The collaborative group has been collecting samples and tracking a group of patients for more than three years now. The data suggests that changes in NfL levels measured in the blood do match up to those found in CSF as the disease progresses. Further, Malaspina and team suggest that high blood NfL levels may correlate with survival time with ALS; meaning that the higher the levels, the longer the survival.
Turner followed Malaspina with additional research from the collaborative, which used magnetic resonance imaging (MRI) technology to attempt to corroborate this data. Looking at the white matter in PALS’ brains, Turner and his team determined the fractional anisotrophy in the corticospinal tract, and found that it correlates with disease progression- further suggesting that NfL levels may be a useful biomarker in ALS.
Following the tag-team event, Bowser took to the podium and offered a different view of neurofilament measurement in ALS. His teams at both the Barrows Institute and his spin-off Iron Horse Diagnostics have been seeking to validate earlier published work suggesting that neurofilament heavy chain (NfH) may be a more appropriate biomarker for ALS, specifically as a diagnostic tool. Bowser has been developing an assay, or test, to measure the presence of NfH in biological samples with the idea that it could be used to speed up the diagnostic process. On average it takes more than a year to diagnose ALS, generally because it is a process of excluding all other possible disorders. This presents a major problem for patients, their attending medical teams, as well as researchers seeking to develop treatments; by the time a person is diagnosed, their disease has progressed significantly.
To attempt to address this issue, Bowser conducted, in partnership with NEALS, a prospective validation study of 126 CSF and 204 plasma samples from 23 different states or provinces in US and Canada. The samples were sent blind to Bowser’s lab, and his team applied their assay to measure the level of NfH in the sample to determine if it was from a PALS or a healthy volunteer. His team failed to identify only four PALS in the CSF samples (92% specificity) with slightly lower efficacy in the plasma samples. Bowser and his team are focused on improving the assay and have already created a modified version which has greater specificity, especially in identifying NfH levels in plasma. However, in closing, and during questioning, he suggested that the test isn’t ready for primetime use in the clinic, and that further work needs to be done to take it from an “academic adventure to industry standards.”